
Risk-Adjusted Orthopaedic Outcomes Enable Fair Comparisons
In the current era of health care reform, cost containment, and the growing focus on the value of care provided, high quality data on the results of orthopaedic care will be critically important (and may soon be demanded) down to the level of the individual institution and even surgeon.
According to David G. Lewallen, MD, Professor of Orthopaedic Surgery, Consultant in the Department of Orthopaedic Surgery, Mayo Clinic, and American Joint Replacement Registry (AJRR) Medical Director: "The availability of risk-adjusted national benchmark data will be increasingly important in fairly interpreting such information and is best developed from large representative datasets that span all age groups and demographics like the AJRR."
Donald Fry, MD, MPA Healthcare Solutions, said, "Many surgeons and quality officers point to their perception that they have the sickest patients to explain suboptimal results or bolster good performance." He added, "There is no question that an accurate interpretation of outcomes and costs cannot be made without an objective measurement of risk adjustment. It is the science of separating the effect of patient characteristics from the effect of care delivered on cost or clinical outcomes."
The Value of a Predictive Risk Adjustment Model
Dr. Fry emphasized, "In order to build a predictive risk adjustment model a list of patient variables must be identified and weighted. Each variable 'weight' represents their influence on one specific adverse outcome or cost that is being studied. These patient characteristics or variables are present when care begins."
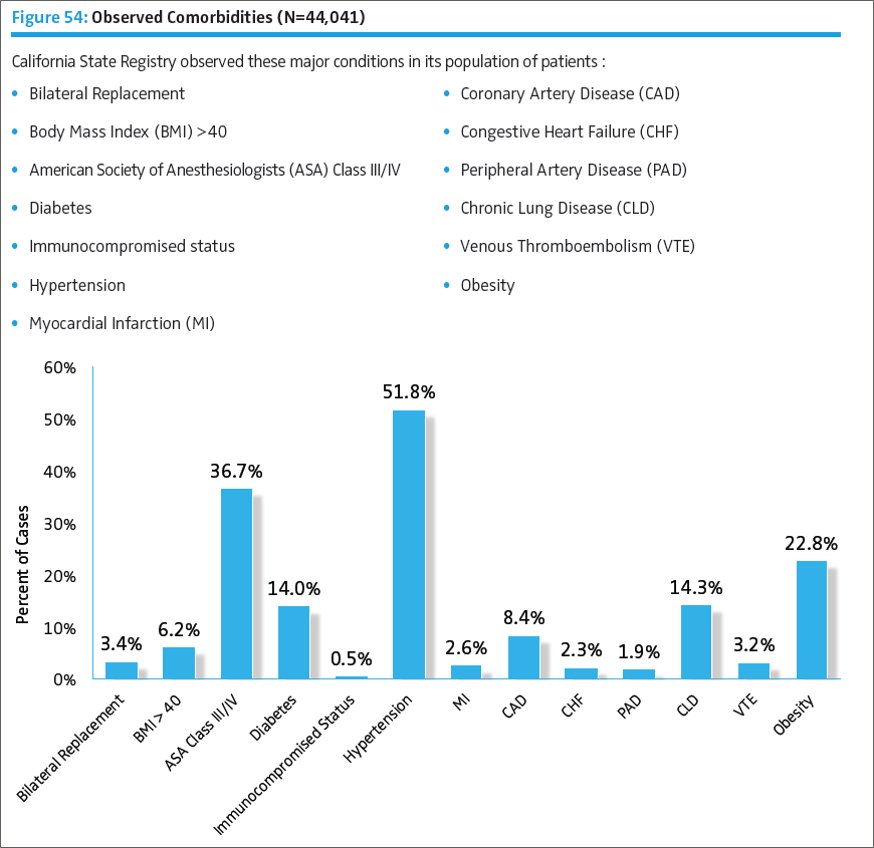
Participation in AJRR can help build the national dataset providers need to effectively judge physicians' individual performance and improve the care they provide. By driving improvements in hospital/clinical site-based care processes, perioperative management, surgical practices, and implant design and performance, it is possible to further enhance patient outcomes. At the same time, the resulting data can help document the dramatic improvement in health status and quality of life that the majority of arthroplasty patients enjoy. Risk-adjusted data can also assist in defending appropriate reimbursement and in meeting the requirements of value-based programs like the Medicare Acute Care Episode (ACE), Bundled Payments for Care Improvement (BPCI), Comprehensive Care for Joint Replacement (CJR), Bundled Payments for Care Improvement - Advanced (BCPI-A), Physician Quality Reporting System (PQRS), Merit-based Incentive Payment System (MIPS), and Medicare Access and CHIP Reauthorization Act of 2015 (MACRA). In doing so, appropriate access to arthroplasty care for patients may be further protected. The California State Registry, part of AJRR, has been collecting patient variables for predictive modeling for some time. For example, the California State Registry observed the major conditions below in its population of patients.
The 2018 AJRR Collection Model Will Include a Full Range of Level II Data
By the second quarter of 2018, AJRR will provide updated data specifications with a finalized Post-Op Complication Layout. Overall, AJRR will collect three levels of data and will report risk-adjusted longitudinal data and benchmarking accordingly. The goal of AJRR benchmarking is to incorporate Level II risk-adjusted data to enable registry participants to accurately benchmark their outcomes and costs against the country, a region, the participant's historical performance, or other desired reference groups.
AJRR Data Collection Model: Where We Are Now
Current Specifications - Version 7/13/17, Three File Layouts
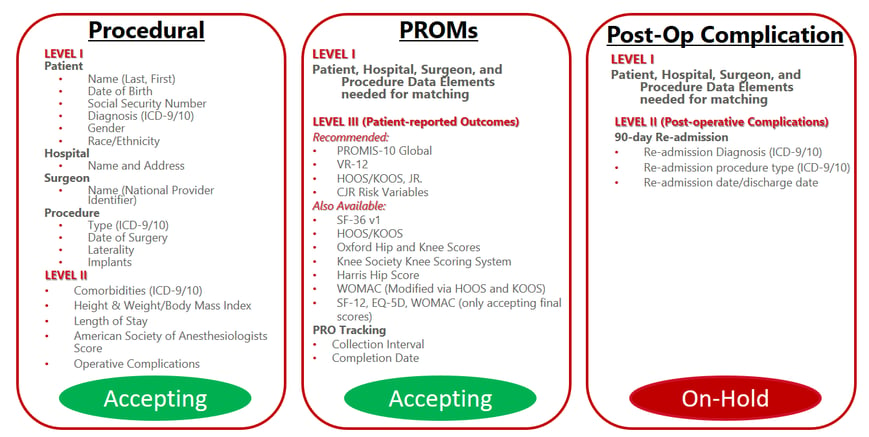

AJRR Data Collection Model: Where We Are Going
The Q2 2018 release of data specifications will: 1) update the data dictionary, 2) introduce minor changes to the Procedural and Patient-Reported Outcome Measures (PROMs) Layout (change the Control Log), 3) revise the Post-Op Complication Layout.
Summary
The AJRR collection model involves required Level I procedural data (patient, hospital, surgeon, implant, etc.) and soon-to-be-required Level II comorbidity and complication data. Level II data, when subject to risk adjustment, results in more meaningful comparative analysis. Data on any reoperations or revisions are collected as subsequently reported to the AJRR and are linked back to the original procedure and patient. Alternatively, this information can be collected later from large claims database matching or reports. The reporting of Level III patient-reported outcome (PRO) data by AJRR participants is currently optional with any of an array of commonly used validated measures accepted and reported back by the Registry for use in internal quality improvement or any external quality reporting requirements like the Centers for Medicare & Medicaid Services (CMS) CJR program. The table to the right shows AJRR Level II Core Data Elements.
Conclusion
Adverse outcomes are known to occur in the experience of all clinicians and hospitals. Risk-adjusted benchmarking of hospital performance, through registries like AJRR, permits the identification of adverse events that may be preventable. Areas in need of improved outcomes, or conditions where costs are greater on a risk-adjusted basis, should become the focus of care redesign. This will help ensure better patient outcomes in the future, lower costs, and resource conservation.
Recommended reading: My Patients Are Sicker Than Other Patients by Donald Fry, MD, MPA Healthcare Solutions, December 2017.
Be sure to leave a comment in the form below!

